News Is it possible to predict the result of an operation for lumbar disc herniation?
Our spine research team has developed a prognosis tool to predict the result of surgery for spinal disc herniation. This means that patients are given a realistic assessment of what they can expect from an operation.
Not every case of lumbar disc herniation (herniated disc) requires surgery. Depending on the extent to which the patient is suffering or in the event that the herniated disc is putting the nerves under so much pressure that the patient is already experiencing dysaesthesia or symptoms of paralysis, surgery is on the cards. But how much improvement can an operation bring about? What can the patient expect from the procedure? This is where a new type of prognosis tool comes in. It shows how the result of an operation will pan out in all likelihood, depending on a range of individual factors.
The prognosis tool was developed by our spine research team and a recent study has been published on it in collaboration with the University of Bern. The results show that it is indeed possible to predict the success of a decompression operation in the event of lumbar disc herniation using the prognosis tool.
Patient information and realistic expectations
The model is based on patient-specific data which was gathered from over 1200 former Schulthess Klinik patients before and after the operation. It showed how various factors such as age, gender, general health, primary symptoms, level of pain, functional impairments, etc. have a significant influence on the result of an operation. This patient data is used for calculation. The algorithm calculates the intensity of back and/or leg pain to be expected as well as the internationally recognised COMI value (multidimensional Core Outcome Measures Index), which was also developed at the Schulthess Klinik, 12 months after surgery. The COMI is a subjective patient-related score and, in addition to the level of pain, also includes back function, symptom-specific well-being, quality of life and disability.
As a result, an individual value with an expectancy range is calculated based on the comprehensive Schulthess Klinik database of patients with the same influencing factors. This value helps doctors to provide realistic and honest information to patients and allows patients to have reasonable expectations of the result of an operation.
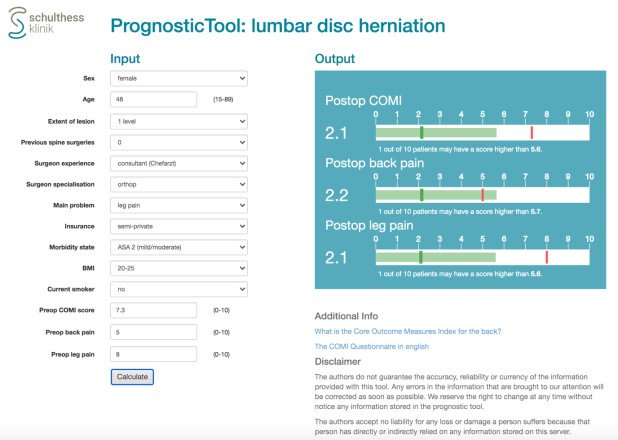
Long-term outcome research
For over 16 years, the Schulthess Klinik has documented the results experienced by its patients who underwent spinal surgery and therefore has a volume of data that is unique throughout Switzerland that supports these predictions. The data is also part of Spine Tango, EUROSPINE’s international spine registry.
This prognosis tool is now being tested further and similar tools for other diseases of the spinal column are in the pipeline. The tool is already available to all medical practitioners for research purposes and also to interested patients. Completing the COMI patient survey is a requirement for the analysis.

