Research as a driver of quality

Research is one of the key ways we advance our quality. Around 40 research associates at Schulthess Klinik work closely with doctors and international partners to keep improving treatment outcomes and quality of life for our patients.
Hip and knee surgery: innovative techniques, proven benefits
The research carried out in our Hip and Knee Surgery department focuses on further refining established procedures and critically evaluating new methods. The aim is to make treatments less invasive whilst ensuring reliable outcomes for patients.
Hip replacement: a small incision with measurable benefits
For hip replacement surgery, Schulthess Klinik has for many years employed a surgical technique involving a very small incision that follows the skin’s natural anatomical tension lines. The so-called “bikini” approach yields a better cosmetic result than if the incision were made parallel to the leg axis.
Our new study now also shows that this approach spares muscles and preserves an important blood vessel that supplies the surrounding musculature. Muscle health is better maintained, and swelling and discomfort in the hip area are reduced. In addition, the function and safety of the procedure remain at the same high level. For patients, this means less stress, a short stay in hospital and a quick return to physical activity, whilst still enjoying outstanding treatment outcomes.
Knee surgery: new cartilage therapy proven effective in comparison study
The development of new surgical methods in knee surgery also focuses on patients’ quality of life and freedom of movement. Two studies investigated the relatively new method of minced cartilage implantation (MCI) for the treatment of cartilage damage. In this procedure, the patient’s own cartilage tissue is mechanically minced, mixed with processed autologous blood and re-implanted in a single operation. MCI was compared with established treatment methods such as microfracturing, which is particularly suitable for less extensive, clearly defined cartilage damage, and autologous chondrocyte implantation, which requires two surgical procedures and is therefore more complex and expensive.
The studies show that two years after the procedure, patients undergoing MCI achieve results that are just as good as those yielded by established treatment methods. Pain is reduced and function improves. MCI thus expands therapeutic options, particularly for young and active people with cartilage injuries.
Both research projects demonstrate how evidence-based development works: it improves existing procedures and provides certainty for treatment decisions regarding knee and hip problems.
Spine surgery: avoiding subsequent operations
If a herniated disc recurs at the same site following disc surgery, surgeons – and patients too – face an important decision: will another decompression operation, in which only part of the intervertebral disc is removed, be sufficient? Or does it make more sense to permanently stabilise the affected vertebral segment via a procedure known as fusion?
In a repeat decompression operation, only the part of the intervertebral disc that is protruding, pressing on the nerves and thus causing the symptoms is removed specifically. The rest of the disc is preserved. In fusion surgery, on the other hand, the damaged intervertebral disc is removed completely. The two adjacent vertebrae are then connected together using screws and rods so that they grow (fuse) together, meaning the section is permanently stabilised.
Significantly lowering risk of a third operation
Our team analysed data from 450 patients who had undergone surgery for a second herniated disc. The study compared decompression surgery with spinal fusion. The results show that both procedures provide similar levels of relief from symptoms. However, the risk of a further – and thus third – operation differed significantly: following a decompression operation, around 37% of the patients affected required further surgery later on, whereas after fusion, the figure was only around 16%.
This finding helps us to plan treatments more effectively. Our clear aim is to avoid further operations wherever possible and to ensure stable long-term outcomes.
The study was awarded the Award of Excellence at the 2025 Annual Congress of the Swiss Society of Spinal Surgery (SGS).

Shoulder and elbow surgery: insights for better decisions
Research in our Shoulder and Elbow Surgery department focuses on areas where new findings can significantly improve treatment. The focus is on issues that are relevant to patients in their day-to-day lives – from pain reduction and improved function to a realistic assessment of treatment success.
Good results – whether on the left or right
Does it matter which shoulder is operated on? Specifically, is it the one you use most in your daily life (dominant shoulder) or the less favoured one? In a large registry study, our team, together with the Hospital for Special Surgery (HSS) in New York, investigated precisely this question: whether a joint replacement on the dominant shoulder leads to better outcomes than on the non-dominant side. Data relating to more than 2,100 patients who underwent total shoulder replacement were analysed. The results show that twelve months after the operation, pain reduction, function and satisfaction are excellent overall, regardless of whether the dominant or non-dominant shoulder was operated on. Arm dominance did not prove to be a clinically relevant influencing factor.
The aim of this joint project is to collate this large volume of patient data in order to further improve treatment outcomes. These findings are particularly valuable for pre-operative consultations. They help to set realistic expectations and give patients confidence in their decision-making.
The study was led by Prof. Dr. med. Markus Scheibel and Dr phil. Asimina Lazaridou from Schulthess Klinik and Dr. Lawrence V. Gulotta and Dr. Jashvant Poeran from HSS.
Personalised shoulder surgery instead of a one-size-fits-all approach
Under the title “One size does not fit all,” the research team led by PD Dr. med. Florian Freislederer investigated the influence of age, gender, height and body mass index on the outcomes of shoulder replacement surgery. The analysis showed that these factors need to be taken into account when choosing a prosthesis in order to achieve better results. If the prosthesis is tailored to these individual patient characteristics, pain can be reduced and function and mobility improved.
Hand surgery: when research reduces the need for surgery
Research in hand surgery aims to make treatments more precise and effective – not through optimised procedures, but through better decision-making.
Minimally invasive treatment of the thumb carpometacarpal joint
A clinical study conducted by our Hand Surgery department shows that, in many cases of osteoarthritis of the thumb carpometacarpal joint, less is more. Contrary to previous practice, additional surgery on the thumb metacarpophalangeal joint is often not necessary to correct hyperextension. The use of a modern thumb carpometacarpal joint prosthesis alone restabilises the metacarpophalangeal joint.
This finding is changing treatment standards for osteoarthritis of the thumb carpometacarpal joint and helps to plan procedures in a more targeted manner in line with the Smarter Medicine principle and avoid unnecessary operations.

AI X-ray analysis
At the same time, the Hand Surgery department is driving forward innovative research initiatives. A doctoral project is currently underway in collaboration with ETH Zurich to investigate how artificial intelligence can automatically analyse X-ray images of the thumb carpometacarpal joint, complementing the assessment made by specialists. This is intended to help to assess the severity of osteoarthritis more consistently, plan operations more precisely and identify post-operative complications at an early stage.
The PhD research project is being conducted by Luca Häfliger at Schulthess Klinik. It combines clinical questions arising from day-to-day treatment with data-based analysis and state-of-the-art technology.
Human Performance Lab: understanding the human body in motion
X-rays, demographic data, information from examinations and patient questionnaires provide important information when it comes to choosing treatment. However, they offer only limited insight into how patients actually move in day-to-day life. This is precisely where research in the Schulthess Klinik’s Human Performance Lab comes in.
Objectively recording movement
In the Human Performance Lab, movements are precisely measured. Patients perform day-to-day or athletic movements while cameras record their movements and force plates register the load when walking or jumping. This creates a detailed picture of how the hips, legs and torso actually behave – far beyond what a static image can show.
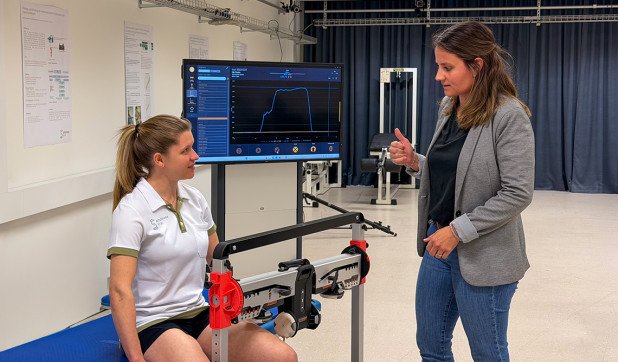
In 2025, the research team systematically worked on establishing a comprehensive database of movement analyses relating to hip impingement. Hip impingement is a deformation of the hip that painfully restricts mobility and has many different treatment options. The aim of the database is to improve the decision-making basis for choosing the best treatment and to enable more realistic assessment of expectations. The latest results show that treatment outcomes can be predicted more accurately by including these movement data.
A complement to outcome research
The findings underline the value of clinical movement analysis as a complement to established outcome research. While questionnaires describe how patients feel, the Human Performance Lab reveals how they move. This combination opens up new opportunities for more targeted treatment planning, avoiding wrong decisions and better assessing the benefits of a particular treatment.
Results presented at the 2025 Annual Meeting of the European Society for Movement Analysis in Adults and Children.